DIGITAL BIOMARKERS | OLDER ADULTS | REMOTE PATIENT MONITORING | NON-INVASIVE MONITORING

DESIGNING A MONITORING SERVICE FOR POST-STROKE DYSPHAGIA PATIENTS
YONSEI HCI LAB (PI: Professor Jinwoo Kim)
ROLE
-
Undergraduate Research Intern
-
Research Team Lead & Qualitative Interviewer
DESCRIPTION
I became interested in doing user research for digital healthcare after this project. As the research team lead, I was in charge of the user interview and formative study process to develop a prototype of a smartphone application to help the monitoring process of patients suffering from dysphagia as a side effect of their stroke.
TEAMMATES
Gayeon Lee, Wanchen Wu, Nahyeon Yoon
TIMELINE
Jan 2025 - Feb 2025
RESEARCH METHODS
Semi-structured interviews
TARGET USERS
-
Caregivers of post-stroke dysphagia patients
-
Post-stroke dysphagia patients
TOOLS
Figma
PROJECT INTRODUCTION
This project is based on the idea of using voice biomarkers to monitor the recovery process of post-stroke dysphagia patients.
After going through a vocalization test and a self-questionnaire, users can track and monitor their recovery process, as well as view resources that may help them recover.
FINAL PROTOTYPE DEMO
3rd iteration
PROBLEM STATEMENT
Post-Stroke Dysphagia Patients
Struggle to Recover Due to
Difficulty of Monitoring
Post-stroke dysphagia is a common complication of acute stroke and is associated with increased mortality and morbidity. Although most patients recover naturally, 11-13% remain dysphagic after 6 months. Patients often struggle to follow through the recovery process without constant help from a physician or a therapist.
Centers for Disease Control and Prevention. (2025, May 26). Data and statistics on autism spectrum disorder. https://www.cdc.gov/autism/data-research/index.html
Zablotsky, B., Black, L. I., Maenner, M. J., Schieve, L. A., Danielson, M. L., Bitsko, R. H., Blumberg, S. J., Kogan, M. D., & Boyle, C. A. (2019). Prevalence and trends of developmental disabilities among children in the United States: 2009-2017. Pediatrics, 144(4), e20190811. https://doi.org/10.1542/peds.2019-0811
World Health Organization. (2025, September 16). Autism spectrum disorders. https://www.who.int/news-room/fact-sheets/detail/autism-spectrum-disorders
Stagg, S. D., & Belcher, H. (2019). Living with autism without knowing: receiving a diagnosis in later life. Health Psychology and Behavioral Medicine, 7(1), 348–361. https://doi.org/10.1080/21642850.2019.1684920
Hanna, J., Gates, J. A., & Hull, L. (2022). Mental health and social difficulties of late-diagnosed autistic adults: A narrative review. Autism, 26(3), 555–570. https://doi.org/10.1177/1362361320979182
What Is Dysphagia?
Dysphagia is a medical condition that includes both difficulty swallowing, or food entering the larynx or trachea by mistake (aspiration).
Chilukuri, P., Odufalu, F., & Hachem, C. (2018). Dysphagia. Missouri medicine, 115(3), 206–210.
Coffey, M., McDermott, S., & O’Beirne, J. (2020). Dysphagia in neurological diseases: Epidemiology, assessment, and management. Neurological Sciences, 41(8), 2131–2137. https://doi.org/10.1007/s10072-020-04495-2
American Speech-Language-Hearing Association. (n.d.). Adult dysphagia. Retrieved October 14, 2025, from https://www.asha.org/practice-portal/clinical-topics/adult-dysphagia/
Patel, D. A., & Krishnaswami, S. (2023). Dysphagia. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK559174/
Labeit, B., Michou, E., Trapl-Grundschober, M., Suntrup-Krueger, S., Muhle, P., Bath, P. M., et al. (2023). The assessment of dysphagia after stroke: State of the art and future directions. The Lancet Neurology, 22(9), 858–870. https://doi.org/10.1016/S1474-4422(23)00153-9
Symptoms of Dysphagia
-
Sensation of food being stuck in the throat or chest
-
An increased number of swallows is required
-
Coughing, choking, or gagging during swallowing attempts
-
Drooling and difficulty controlling saliva
-
Hoarseness and voice changes
-
Nasal regurgitation of food or liquids
-
Frequent throat clearing
-
Need for liquid to wash down food
-
Significant time required to complete meals
Chilukuri, P., Odufalu, F., & Hachem, C. (2018). Dysphagia. Missouri medicine, 115(3), 206–210.
Coffey, M., McDermott, S., & O’Beirne, J. (2020).
Patel, D. A., & Krishnaswami, S. (2023). Dysphagia. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK559174/
Sebastian, S., Nair, P. G., Thomas, P., & Tyagi, A. K. (2015). Oropharyngeal Dysphagia: neurogenic etiology and manifestation. Indian journal of otolaryngology and head and neck surgery : official publication of the Association of Otolaryngologists of India, 67(Suppl 1), 119–123. https://doi.org/10.1007/s12070-014-0794-3
Labeit, B., Michou, E., Trapl-Grundschober, M., Suntrup-Krueger, S., Muhle, P., Bath, P. M., et al. (2023). The assessment of dysphagia after stroke: State of the art and future directions. The Lancet Neurology, 22(9), 858–870. https://doi.org/10.1016/S1474-4422(23)00153-9
Post-Stroke Dysphagia
vs. Dysphagia
Post-stroke dysphagia (PSD) represents a specific subset of neurogenic dysphagia with distinct characteristics and mechanisms. While general dysphagia encompasses various cuases, post-stroke dysphagia has unique features related to cerebrovascular damage.
Post-stroke dysphagia results from specific disruptions in brain areas controlling swallowing, including the sensorimotor cortex, brainstem swallowing centers, and connecting neural pathways. The recovery process involves neuroplastic compensatory mechanisms, particularly increased activity in the unaffected hemisphere.
Chilukuri, P., Odufalu, F., & Hachem, C. (2018). Dysphagia. Missouri medicine, 115(3), 206–210.
Coffey, M., McDermott, S., & O’Beirne, J. (2020).
Patel, D. A., & Krishnaswami, S. (2023). Dysphagia. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK559174/
Sasegbon, A., Cheng, I., & Hamdy, S. (2025). The neurorehabilitation of post-stroke dysphagia: Physiology and pathophysiology. The Journal of physiology, 603(3), 617–634. https://doi.org/10.1113/JP285564
González-Fernández, M., Ottenstein, L., Atanelov, L., & Christian, A. B. (2013). Dysphagia after Stroke: an Overview. Current physical medicine and rehabilitation reports, 1(3), 187–196. https://doi.org/10.1007/s40141-013-0017-y
Labeit, B., Michou, E., Trapl-Grundschober, M., Suntrup-Krueger, S., Muhle, P., Bath, P. M., et al. (2023). The assessment of dysphagia after stroke: State of the art and future directions. The Lancet Neurology, 22(9), 858–870. https://doi.org/10.1016/S1474-4422(23)00153-9
Impact of Post-Stroke Dysphagia on Patients
Malnutrition
-
Malnutrition in approximately 51% of patients (2.72-fold increased risk compared to those without swallowing difficulties).
Aspiration
& Respiratory Issues
-
Aspiration: Approximately 52% of patients with dysphagia.
-
Increased risk of aspiration pneumonia by 17% compared to non-dysphagic patients.
Healthcare Burden
-
Patients face 1.82 times higher risk of pneumonia readmissions
-
5.07 times higher risk of aspiration pneumonia readmissions
Increased Mortality Risk
& Complications
-
Death rates exceeding 30% in dysphagic stroke survivors
-
Increased risk of neurological impairment, respiratory infections, and urinary infections
Lower Quality of Life
-
41% experience anxiety or panic during mealtimes.
-
Social Isolation: More than one-third avoid eating with others due to swallowing difficulties
Post-stroke Fatigue and Depression Risks
-
Chronic fatigue for over 80%, compared to 50% of all stroke patients
-
Increased likelihood of depression and anxiety symptoms
Karisik, A., Moelgg, K., Buergi, L., et al. (2025). Dysphagia increases the risk of post-stroke fatigue. European Journal of Neurology, 32, e16570. https://doi.org/10.1111/ene.16570
Wang, Z., Li, J., Luo, D., Zeng, X., Guo, S., & Wang, T. (2025). Post-stroke dysphagia: Neurological regulation and rehabilitation strategies. Biomedical Science and Technology, 34(1), 29–45. https://doi.org/10.5582/bst.2025.01029
Xu, X., Wang, Z., Zhang, J., & Song, M. (2025). Post-stroke dysphagia: Identifying the evidence missing. Frontiers in Medicine, 12, Article 1494645. https://doi.org/10.3389/fmed.2025.1494645
asegbon, A., Cheng, I., & Hamdy, S. (2025). The neurorehabilitation of post-stroke dysphagia: Physiology and pathophysiology. The Journal of physiology, 603(3), 617–634. https://doi.org/10.1113/JP285564
González-Fernández, M., Ottenstein, L., Atanelov, L., & Christian, A. B. (2013). Dysphagia after Stroke: an Overview. Current physical medicine and rehabilitation reports, 1(3), 187–196. https://doi.org/10.1007/s40141-013-0017-y
Karunaratne, T. B., Clavé, P., & Ortega, O. (2024). Complications of oropharyngeal dysphagia in older individuals and patients with neurological disorders: insights from Mataró hospital, Catalonia, Spain. Frontiers in neurology, 15, 1355199. https://doi.org/10.3389/fneur.2024.1355199
VASCage – Center on Clinical and Translational Stroke Research. (2024, December 8). Swallowing difficulties after stroke burden mental health. https://vascage.at/swallowing-difficulties-after-stroke-burden-mental-health/
USER INTERVIEWS
Before designing our application, my team and I were able to interview a total of six guardians of patients and two occupational therapists regarding the difficulties related to the monitoring process of post-stroke dysphagia.
It's Difficult
to Stay Motivated
(KOR → ENG Translated) “My father was admitted to the ICU and was diagnosed with dysphagia. ... A caregiver was absolutely necessary for rehabilitation, but hiring one was too expensive.
It would be important for patients to recognize their own symptoms for faster recovery.
If rehabilitation lasts beyond three to four months, it becomes very tough and motivation disappears.”
— Son of post-stroke dysphagia patient (P3)

(KOR → ENG Translated) My mother was diagnosed with a left-side stroke this January. She has swallowing difficulties and speech impairment. She experiences pain when swallowing medicine or drinking water due to her swallowing problems. Breathing is difficult for her, and her speech ability is limited. She told me that she feels extremely anxious and restless.
Although she is willing to go through rehabilitation, her emotional fluctuations sometimes discourage her.
She currently has about four hours of rehabilitation daily, including physical and speech therapy.
— Daughter of post-stroke dysphagia patient (P6)
.png)
It's Difficult to Visit Hospitals Often
(KOR → ENG Translated) “I have seen quite a number of patients who found it difficult to continue their recovery process, especially after being discharged from the hospital. I have seen cases where patients had to visit hospitals that are 5 hours away from them, which makes it difficult for them to track their recovery process often.
Not a lot of patients can visit the hospital often, mostly due to physical constraints.
In turn, this often makes the recovery process longer and more painful.
— Occupational Therapist with experience treating post-stroke dysphagia patients (P5)
STAKEHOLDER MAPPING
Through our literature review and interviews, we discovered that the guardians of post-dysphagia patients (often their children), are directly involved in the problem. Hence, we must factor them in the process of designing the application.
_edited.png)
HOW MIGHT WE...
Painpoint 1
Users have low motivation and poor adherence to rehabilitation exercises, leading to slow or little improvement.
How Might We...
Motivate patients to consistently engage in rehabilitation and make progress in recovering their swallowing function.
Painpoint 2
Users have difficulty accessing affordable, consistent care for post-stroke dysphagia.
How Might We...
Make high-quality caregiving and support for dysphagia more accessible and affordable for patients and families.
Painpoint 3
Users face emotional and social isolation stemming from swallowing difficulties and lengthy recovery.
How Might We...
Help dysphagia patients and caregivers feel more supported and socially connected during recovery.
REASEARCH QUESTION
“What if... we use voice biomarkers
as a non-invasive method to monitor dysphagia in post-stroke patients?”
THE CORE IDEA
A Remote Monitoring Service to Track The Recovery Process of Post-Stroke Dysphagia Patients
KEY FEATURES
Voice Detection for Remote Monitoring
For a non-invasive yet convenient monitoring process
K-EAT 10 Questionnaire
To quickly and accurately screen for the risk of dysphagia
Visualizing Recovery Process
To streamline the diagnosis process by providing data that medical experts can use to add to the official diagnosis
COMPETITIVE BUSINESS ANALYSIS
Currently, most studies focus on giving treatment instead of an assessment.

Kim, H., Cho, N., Kim, J., Kim, K., Kang, M., Choi, Y., Kim, M., You, H., Nam, S., & Shin, S. (2020). Implementation of a home-based mHealth app intervention program with human mediation for swallowing tongue pressure strengthening exercises in older adults: Longitudinal observational study. JMIR mHealth and uHealth, 8(10), e22080. https://doi.org/10.2196/22080
Malandraki, G. A., Arkenberg, R. H., Mitchell, S. S., & Malandraki, J. B. (2021). Telehealth for Dysphagia Across the Life Span: Using Contemporary Evidence and Expertise to Guide Clinical Practice During and After COVID-19. American journal of speech-language pathology, 30(2), 532–550. https://doi.org/10.1044/2020_AJSLP-20-00252
Wang, Z., Dai, X., & Wu, C. (2023). Effect of an individualized digital coaching program on swallowing function in stroke patients. Acta neurologica Belgica, 123(3), 963–969. https://doi.org/10.1007/s13760-022-02153-2
Son, I., Shim, H.-Y., Lee, S.-C., Kim, H.-G., Park, M.-S., & … Lee, J.-H. (2023). Non-invasive way to diagnose dysphagia by training deep learning model with voice spectrograms. Biomedical Signal Processing and Control, 86, 105259. https://doi.org/10.1016/j.bspc.2023.105259
Zhang, J.-R., Wu, Y.-E., Huang, Y.-F., Zhang, S.-Q., Pan, W.-L., Huang, J.-X., & Huang, Q.-P. (2023). Effectiveness of smart health–based rehabilitation on patients with poststroke dysphagia: A brief research report. Frontiers in Neurology, 13, 1110067. https://doi.org/10.3389/fneur.2022.1110067
INFORMATION ARCHITECTURE

UI DESIGN REFERENCES FOR PATIENTS RECOVERING FROM A STROKE

Font Family: Inter
Typography
and Readability
Use large font sizes, high contrast ratios between text and background, and sans serif fonts for readability.
.png)
Progress and Achievement
Stroke rehabilitation requires sustained engagement over long periods.
Include visible progress tracking with both short and long-term goals,
and historical data visualization to show improvement trends.
#007AFF
#5CB388
#FFC859
Color and
Visual Elements
Implement consistent color-coding systems, text labels, and clear distinction between headings
and body text.

Cognitive Load Management
To reduce cognitive fatigue, use simple interfaces without complex background images or flashing elements. Support memory limitations by minimizing information that must be remembered between screens.
5.png)
Information
Processing
Use simple, direct language with short sentences. Present one primary task per screen to avoid cognitive overload.

Visual and Layout Guidelines
Ensure high contrast ratios between text and background colors. Need generous white space to reduce visual clutter and consistent layout patterns to support recognition over recall.
Cavuoto, L. A., Subryan, H., Stafford, M., Yang, Z., Bhattacharjya, S., Xu, W., & Langan, J. (2018). Understanding User Requirements for the Design of a Home-Based Stroke Rehabilitation System. Proceedings of the Human Factors and Ergonomics Society ... Annual Meeting. Human Factors and Ergonomics Society. Annual meeting, 62(1), 1037–1041. https://doi.org/10.1177/1541931218621239
Magnusson, C., Anastassova, M., Paneels, S., Rassmus-Gröhn, K., Rydeman, B., Randall, G., Ortiz Fernandez, L., Bouilland, S., Pager, J., & Hedvall, P. O. (2018). Stroke and Universal Design. Studies in health technology and informatics, 256, 854–861.
Magnusson, C., Anastassova, M., Paneels, S., Rassmus-Gröhn, K., Rydeman, B., Randall, G., Ortiz Fernandez, L., Bouilland, S., Pager, J., & Hedvall, P. O. (2018). Stroke and Universal Design. Studies in health technology and informatics, 256, 854–861.
Cavuoto, L. A., Subryan, H., Stafford, M., Yang, Z., Bhattacharjya, S., Xu, W., & Langan, J. (2018). Understanding User Requirements for the Design of a Home-Based Stroke Rehabilitation System. Proceedings of the Human Factors and Ergonomics Society ... Annual Meeting. Human Factors and Ergonomics Society. Annual meeting, 62(1), 1037–1041. https://doi.org/10.1177/1541931218621239
Health Care Providers Association. (2024, December 9). Making information accessible for people with Aphasia: A New Guide. HCPA. https://www.hcpa.info/health/making-information-accessible-for-people-with-aphasia-a-new-guide/
World Wide Web Consortium. (2020, December 11). Design guide | Making content usable for people with cognitive and learning disabilities. W3C Working Draft. https://www.w3.org/TR/2020/WD-coga-usable-20201211/design_guide.html
Svensson, P. (2025). Usability and accessibility in mHealth stroke apps. Informatics in Medicine Unlocked, 53, 101616. https://doi.org/10.1016/j.imu.2025.101616
DESIGNING MONITORING TESTS
We decided to use two different kinds of tests in our application to provide an accurate and helpful monitoring for patients: The voice test and the K-EAT 10.
5.png)
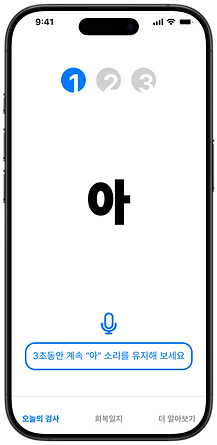
Test with Vowels

Test with Words
Voice Test (Collecting Voice Biomarkers & Analysis with Deep Learning)
Using a deep learning models, this test analyzes standardized vowels and words from post-stroke patients to detect and track their recovery progress.
Research basis: Roldan-Vasco et al. (2021) developed a proof-of-concept model using speech samples from 68 post-stroke patients (40 training, 28 testing), where voice data was segmented into 1,579 audio clips and converted to 6,655 Mel-spectrogram images using established CNN architectures.
Validity evidence: Roldan-Vasco et al. (2021) validated their results against the Toronto Bedside Swallowing Screening Test (TOR-BSST) as the gold standard labeling method, with concurrent assessment by trained speech-language pathologists.
Accuracy metrics: Previous studies, such as Roldan-Vasco et al. (2021), achieved participant-level sensitivity of 89% and specificity of 79% (F1 = 0.81, AUC = 0.91 [95% CI: 0.77-1.05]), with clip-level sensitivity of 71% and specificity of 77% (F1 = 0.73, AUC = 0.80).
Roldan-Vasco, S., Orozco-Duque, A., Suarez-Escudero, J. C., & Orozco-Arroyave, J. R. (2021). Machine learning based analysis of speech dimensions in functional oropharyngeal dysphagia. Computer methods and programs in biomedicine, 208, 106248. https://doi.org/10.1016/j.cmpb.2021.106248
Heo, S., Uhm, K. E., Yuk, D., Kim, B. M., Yun, B., Kim, J., & Lee, J. (2024). Deep learning approach for dysphagia detection by syllable-based speech analysis with daily conversations. Scientific Reports, 14, 20270. https://doi.org/10.1038/s41598-024-70774-z
Park, H.-Y., Park, D., Kang, H. S., Kim, H., Lee, S., & Im, S. (2022). Post-stroke respiratory complications using machine learning with voice features from mobile devices. Scientific Reports, 12, 16682. https://doi.org/10.1038/s41598-022-20348-8
Kim, J.-M., Kim, M.-S., Choi, S.-Y., Lee, K., & Ryu, J. S. (2024). A deep learning approach to dysphagia-aspiration detecting algorithm through pre- and post-swallowing voice changes. Frontiers in Bioengineering and Biotechnology, 12, 1433087. https://doi.org/10.3389/fbioe.2024.1433087
Gugatschka, M., Egger, N. M., Haspl, K., Hortobagyi, D., Jauk, S., Feiner, M., & Kramer, D. (2024). Clinical evaluation of a machine learning-based dysphagia risk prediction tool. European archives of oto-rhino-laryngology : official journal of the European Federation of Oto-Rhino-Laryngological Societies (EUFOS) : affiliated with the German Society for Oto-Rhino-Laryngology - Head and Neck Surgery, 281(8), 4379–4384. https://doi.org/10.1007/s00405-024-08678-x
Enz, V. C. Q., Vaz, A. R. C., Nunes, M. C. A., Rosa, M. O., Nunes, J. A., Marques, J. M., & Santos, R. S. (2022). Accuracy of Acoustic Evaluation of Swallowing as a Diagnostic Method of Dysphagia in Individuals Affected by Stroke: Preliminary Analysis. Dysphagia, 37(4), 724–735. https://doi.org/10.1007/s00455-021-10358-5
Santamato, A., Panza, F., Solfrizzi, V., Russo, A., Frisardi, V., Megna, M., Ranieri, M., & Fiore, P. (2009). Acoustic analysis of swallowing sounds: a new technique for assessing dysphagia. Journal of rehabilitation medicine, 41(8), 639–645. https://doi.org/10.2340/16501977-0384
Saab, R., Balachandar, A., Mahdi, H., Nashnoush, E., Perri, L. X., Waldron, A. L., Sadeghian, A., Rubenfeld, G., Crowley, M., Boulos, M. I., Murray, B. J., & Khosravani, H. (2023). Machine-learning assisted swallowing assessment: a deep learning-based quality improvement tool to screen for post-stroke dysphagia. Frontiers in neuroscience, 17, 1302132. https://doi.org/10.3389/fnins.2023.1302132

K-EAT 10 Self-Questionnaire
The K-EAT-10 is a Korean-adapted, 10-item self-assessment questionnaire, designed to quickly screen for the risk of dysphagia by measuring the severity of swallowing difficulties on a scale from 0 to 40.
Research Basis: The original EAT-10 tool was developed in 2008 by Belafsky et al. and widely translated and validated internationally. It is grounded in patient-reported symptoms that correlate with objective swallowing assessments, such as Flexible Endoscopic Evaluation of Swallowing (FEES) and Videofluoroscopic Swallowing Study (VFSS).
Validity Evidence: The K-EAT-10 has demonstrated high internal consistency (Cronbach’s α = 0.901) and excellent test-retest reliability, confirming that the tool is stable and coherent in its measurement of dysphagia symptoms.
Accuracy Metrics: Meta-analyses assessing EAT-10 screening accuracy across populations indicate that a cutoff score of 3 provides the best balance between sensitivity (85%) and specificity (82%) for detecting dysphagia using FEES or VFSS as gold standards. The area under the receiver operating characteristic curve (AUC) is 0.903 for cutoff 3, indicating excellent overall accuracy.
Belafsky, P. C., Mouadeb, D. A., Rees, C. J., Pryor, J. C., Postma, G. N., Allen, J., & Leonard, R. J. (2008). Validity and reliability of the Eating Assessment Tool (EAT-10). Annals of Otology, Rhinology & Laryngology, 117(12), 919-924. https://doi.org/10.1177/000348940811701210
Min, K. C., & Woo, H. S. (2022). Prevalence and characteristics of dysphagia in community-dwelling elderly using the Korean version of Eating Assessment Tool-10 (K-EAT-10). Korean Journal of Occupational Therapy, 30(4), 61-76. https://doi.org/10.14519/kjot.2022.30.4.06
Jardine, M., Miles, A., & Allen, J. (2021). Self-reported swallowing and nutrition status in community-living older adults. Dysphagia, 36(2), 198-206. 10.1007/s00455-020-10125-y 32385694
Nishida, T., Yamabe, K., Ide, Y., & Honda, S. (2020). Utility of the Eating Assessment Tool-10 (EAT-10) in evaluating self-reported dysphagia associated with oral frailty in Japanese community-dwelling older people. The Journal of Nutrition, Health & Aging, 24(1), 3-8. https://doi.org/10.1007/s12603-019-1256-0
Zhang, P. P., Yuan, Y., Lu, D. Z., Li, T. T., Zhang, H., Wang, H. Y., & Wang, X. W. (2023). Diagnostic Accuracy of the Eating Assessment Tool-10 (EAT-10) in Screening Dysphagia: A Systematic Review and Meta-Analysis. Dysphagia, 38(1), 145–158. https://doi.org/10.1007/s00455-022-10486-6
Zhang, P. P., Yuan, Y., Lu, D. Z., Li, T. T., Zhang, H., Wang, H. Y., & Wang, X. W. (2023). Diagnostic Accuracy of the Eating Assessment Tool-10 (EAT-10) in Screening Dysphagia: A Systematic Review and Meta-Analysis. Dysphagia, 38(1), 145–158. https://doi.org/10.1007/s00455-022-10486-6
Results & Progress Log
-
Visualize the recovery process with charts and graphs.
-
Check detailed feedback for each test and access speech-related functions.
-
View recovery progress over time.
-
Allow patients to perform daily tests at set times for consistent monitoring.
.png)

Resources for Guardians
Read our recommendations for resources that allows both the patient and caregivers for personalized solutions.
Impact
This research directly tackles the significant problem of diagnostic delays. We found that families typically wait about a year for an autism diagnosis. Furthermore, using a multi-modal biomarker approach with AI detection tools, our study contributes to this growing body of evidence supporting digital screening approaches.
Overall, while designing our prototype, we aimed to take a user-centered design approach with extensive stakeholder engagement (including teenagers, parents, and medical experts) to provide a robust framework in developing accessible digital health tools for teenage autistic individuals.
Limitations and Future Research Directions
-
Limited device compatibility (only smartphone prototype)
-
Need for larger-scale validation studies
My Key Takeaways
-
Motivating users is key when designing digital healthcare products. My previous PI told me that the first digital healthcare product in Korea was designed for insomniacs, featuring Cognitive Behavioral Therapy. However, it had problems with user retention, because it could not help the users stay motivated. Whether users would actually be willing to use the product is a key question to ask during the research process. Even if the product includes cutting-edge technology, it will not be relevant if the users are not willing to use it.
-
It can be very tricky to design products for medical conditions where the causes and symptoms can vary significantly per individual. My team and I originally wanted to work on developing a product for post-stroke insomnia, but we had difficulties because we couldn't distinguish between insomnia and post-stroke insomnia to create a product targeted towards post-stroke insomnia patients.
-
Consider levels of cognitive functioning when designing for patients with brain damage. One thing I realized when interviewing guardians was that it is difficult for users to engage with the product if I don't consider their level of cognitive functioning during the design process.